Why Developing Countries Face a Silent Cancer Crisis
Cancer is often perceived as a disease more common in wealthy nations, where lifestyles are more sedentary and populations live longer. However, a quieter and deeply concerning reality is unfolding across many developing countries. Cancer has become a silent crisis—growing steadily, often undetected, and frequently untreated until it reaches advanced stages. Unlike infectious diseases that create sudden outbreaks and visible emergencies, cancer progresses quietly, making it harder to recognize as a public health priority. Yet its impact on families, communities, and healthcare systems is profound.
One of the central reasons for this silent crisis is demographic change. Many developing nations are experiencing longer life expectancy due to improvements in vaccination, sanitation, and control of infectious diseases. As populations age, the number of cancer cases naturally rises because cancer risk increases with age. However, healthcare systems in these countries were historically structured to combat infectious diseases rather than long-term, non-communicable illnesses like cancer.
Limited awareness plays a significant role. In many communities, early warning signs such as persistent cough, unexplained weight loss, abnormal bleeding, or lumps may be ignored or misunderstood. Cultural beliefs, stigma, and fear can prevent individuals from seeking medical attention. Some people associate cancer with death, leading to denial or avoidance instead of early consultation.
Another critical issue is the lack of screening and early detection programs. In high-income countries, routine screening for cancers such as breast, cervical, and colorectal cancer helps identify disease at an early, treatable stage. In contrast, screening services may be unavailable, inaccessible, or unaffordable in low-resource settings. As a result, many patients are diagnosed only when symptoms become severe, reducing survival chances.
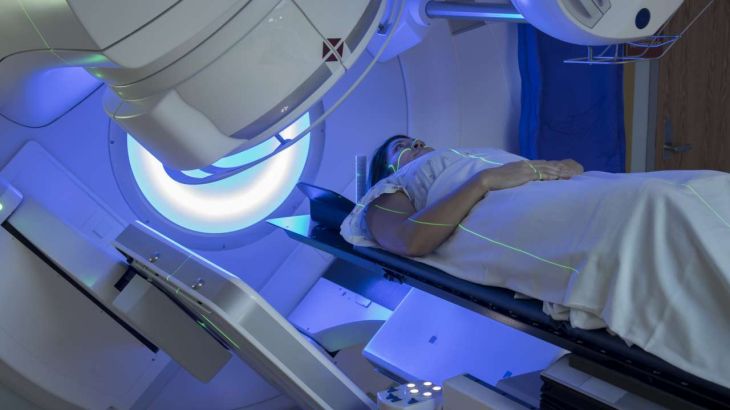
Healthcare infrastructure also presents a challenge. Many developing countries face shortages of trained oncologists, diagnostic equipment, radiotherapy units, and chemotherapy facilities. Rural populations often must travel long distances to access specialized care, creating delays in diagnosis and treatment. Financial constraints further complicate the situation, as cancer treatment can be expensive and prolonged.
Several interrelated factors contribute to this silent cancer crisis:
Limited public awareness and health education about cancer symptoms.
Inadequate screening and early detection programs.
Shortage of specialized healthcare professionals and treatment centers.
High out-of-pocket healthcare expenses.
Cultural stigma and misconceptions surrounding cancer.
Growing exposure to environmental and lifestyle risk factors.
Economic transitions also influence cancer patterns. As developing countries urbanize and adopt more Westernized lifestyles, rates of smoking, processed food consumption, obesity, and physical inactivity increase. These changes contribute to rising cases of lung, colorectal, breast, and other cancers. Tobacco use, in particular, remains a significant driver of cancer burden in many regions due to weaker regulation and marketing controls.
Environmental factors further compound the problem. Rapid industrialization without strict environmental safeguards can increase exposure to air pollution, contaminated water, and hazardous chemicals. Occupational safety standards may be less rigorously enforced, placing workers at higher risk of long-term exposure to carcinogens.
Infectious agents linked to cancer remain more prevalent in developing countries. Certain viruses and bacteria can trigger cancers if left untreated. Limited access to vaccination programs, early treatment, and screening allows these infections to persist, increasing long-term cancer risk. This creates a dual burden: while infectious diseases decline overall, infection-related cancers remain significant.
Financial hardship intensifies the crisis. In many low- and middle-income countries, health insurance coverage is limited. Families often bear the full cost of diagnosis and treatment. The expense of surgery, chemotherapy, or radiation therapy can push households into poverty. Consequently, some patients abandon treatment midway or avoid seeking care entirely.
The psychological and social impact of cancer in developing countries is equally profound. Without adequate support systems, families may struggle emotionally and financially. Caregiving responsibilities often fall on women, affecting employment and education. Children may leave school to help support the household, perpetuating cycles of poverty.
Data collection and cancer registries are often incomplete, contributing to the “silent” nature of the crisis. Without accurate statistics, policymakers may underestimate the true scale of the problem. Underreporting makes it harder to allocate resources effectively or implement national cancer control programs.
Despite these challenges, there are encouraging signs of progress. International collaborations, government initiatives, and nonprofit organizations are working to improve access to screening, treatment, and awareness campaigns. Vaccination programs targeting infection-related cancers and community health education efforts are expanding in many regions.
Prevention remains a powerful tool. Public health measures such as tobacco control policies, clean air regulations, improved sanitation, and promotion of healthy diets can significantly reduce cancer risk. Early detection programs, even low-cost ones such as clinical breast exams or visual inspection for cervical cancer, can make a meaningful difference when implemented widely.
Strengthening primary healthcare systems is crucial. Training frontline health workers to recognize early cancer symptoms and refer patients promptly can bridge gaps in specialized care. Investment in affordable diagnostic technologies and regional cancer centers can also reduce disparities between urban and rural populations.
In conclusion, developing countries face a silent cancer crisis driven by demographic shifts, limited awareness, inadequate healthcare infrastructure, economic challenges, and rising exposure to lifestyle and environmental risks. Unlike infectious outbreaks, cancer does not announce itself dramatically, yet its long-term impact is devastating. Addressing this crisis requires coordinated efforts in prevention, education, early detection, affordable treatment, and health system strengthening. By recognizing cancer as a growing public health priority rather than a distant threat, developing nations can begin to confront and reduce the burden of this silent epidemic.