Lifestyle Role in Cancer Development
Cancer is often viewed as a genetic disease, but genes alone do not tell the whole story. While inherited mutations can increase risk, a significant proportion of cancers are influenced by lifestyle choices and environmental exposures. The way people eat, move, sleep, manage stress, and interact with their surroundings can either protect cells from damage or gradually create conditions that favor the development of cancer. Understanding the link between lifestyle and cancer development helps individuals make informed decisions that reduce long-term health risks.
At the core of cancer development lies cellular damage, particularly damage to DNA. Cells in the body constantly divide, repair themselves, and communicate with neighboring cells. When harmful exposures repeatedly injure cells or interfere with repair systems, mutations can accumulate. Over time, these mutations may disrupt genes that control cell growth and survival, leading to uncontrolled division. Lifestyle habits play a critical role in determining how often such cellular damage occurs and how effectively the body can respond to it.
One of the most significant lifestyle-related risk factors for cancer is tobacco use. Tobacco smoke contains numerous carcinogens—substances capable of causing cancer. These chemicals directly damage the DNA in cells lining the lungs, mouth, throat, and other organs. Repeated exposure overwhelms the body’s repair mechanisms, increasing the likelihood of permanent mutations. Smoking is strongly associated with lung cancer, but it also raises the risk of cancers of the bladder, pancreas, kidney, cervix, and more. Even secondhand smoke can contribute to cellular injury.
Diet is another powerful influence. The foods people consume affect inflammation levels, hormone balance, immune function, and body weight—all of which are linked to cancer risk. Diets high in processed meats, refined sugars, and unhealthy fats may promote chronic inflammation and oxidative stress. Oxidative stress occurs when harmful molecules called free radicals damage cells and DNA. On the other hand, diets rich in fruits, vegetables, whole grains, and legumes provide antioxidants and fiber, which help neutralize free radicals and support digestive health.
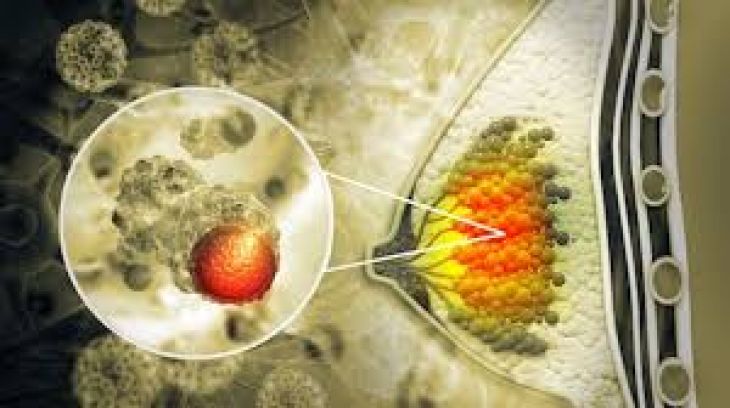
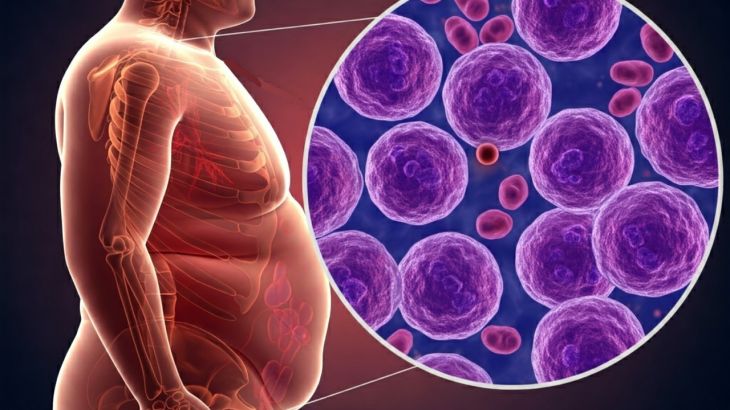
Physical activity also plays a protective role. Regular exercise improves immune surveillance, reduces inflammation, and helps maintain healthy body weight. Excess body fat, particularly around the abdomen, is linked to higher levels of hormones such as estrogen and insulin. Elevated levels of these hormones can stimulate cell growth, increasing the chance that abnormal cells will multiply. Obesity has been associated with cancers of the breast (especially after menopause), colon, endometrium, kidney, and pancreas.
Several key lifestyle factors that contribute to cancer development include:
Tobacco use: Directly damages DNA and promotes chronic inflammation.
Unhealthy diet: High intake of processed foods and low intake of protective nutrients.
Physical inactivity: Contributes to obesity and hormonal imbalance.
Excessive alcohol consumption: Produces toxic byproducts that damage cells and increase cancer risk.
Chronic sun exposure: Ultraviolet (UV) radiation causes direct DNA mutations in skin cells.
Persistent stress and poor sleep: Weaken immune function and disrupt hormonal regulation.
Alcohol consumption deserves special attention. When alcohol is metabolized in the body, it forms acetaldehyde, a toxic compound that can damage DNA and interfere with repair processes. Alcohol also increases estrogen levels and can make it easier for other carcinogens, such as those in tobacco smoke, to enter cells. Regular heavy drinking is associated with cancers of the liver, breast, mouth, throat, and esophagus.
Sun exposure is another lifestyle-related risk factor. Ultraviolet radiation from the sun or tanning devices penetrates skin cells and causes direct DNA damage. If the damage is not properly repaired, mutations accumulate, potentially leading to skin cancers such as melanoma and non-melanoma types. Protective behaviors like wearing sunscreen, protective clothing, and limiting peak sun exposure significantly reduce this risk.
Chronic stress and insufficient sleep may not directly cause cancer, but they influence biological systems that affect cancer development. Long-term stress can increase inflammation and alter hormone levels. Poor sleep disrupts the body’s circadian rhythm, which regulates cell repair and immune activity. Over time, these disruptions may create an environment that supports tumor growth.
Environmental exposures tied to lifestyle choices also matter. Urban air pollution, occupational exposure to chemicals, and indoor pollutants can contribute to cumulative DNA damage. Choosing to use protective equipment at work, ensuring proper ventilation at home, and reducing exposure to harmful chemicals are preventive strategies within individual control.
Importantly, lifestyle factors often interact rather than act alone. For example, smoking combined with heavy alcohol use significantly increases the risk of certain cancers more than either factor individually. Similarly, obesity combined with physical inactivity and poor diet creates a metabolic environment characterized by inflammation, insulin resistance, and oxidative stress—conditions favorable for cancer development.
However, it is equally important to emphasize that lifestyle changes can lower risk. The body possesses remarkable repair and defense mechanisms. When individuals adopt healthier habits, they reduce ongoing cellular injury and strengthen immune responses. For example, quitting smoking begins to lower cancer risk within years. Adopting a balanced diet rich in plant-based foods increases antioxidant intake and supports detoxification processes. Regular physical activity enhances immune function and helps regulate hormones.
Vaccination and preventive healthcare also fall under lifestyle choices. Vaccines against certain viruses, such as human papillomavirus (HPV) and hepatitis B, reduce the risk of virus-related cancers. Regular health screenings allow early detection of precancerous changes before they develop into invasive disease.
It is crucial to recognize that not all cancers are preventable. Some occur despite healthy living due to genetic predisposition or random cellular errors. However, research consistently shows that a substantial percentage of cancer cases worldwide are linked to modifiable risk factors. This means that daily decisions—what to eat, whether to smoke, how active to be—can significantly influence long-term outcomes.
In conclusion, lifestyle plays a profound role in cancer development by shaping the cellular environment in which mutations arise and progress. Habits such as smoking, poor diet, inactivity, excessive alcohol consumption, and unprotected sun exposure increase DNA damage and weaken protective mechanisms. Conversely, balanced nutrition, regular exercise, adequate sleep, stress management, and preventive healthcare strengthen the body’s defenses. Cancer often develops over many years, and lifestyle choices made consistently over time can either accelerate or slow this process. By understanding and modifying these factors, individuals can actively reduce their risk and promote long-term health.