The Link Between Obesity, Insulin Resistance, and Cancer Risk
In recent decades, scientists have increasingly recognized that lifestyle and metabolic health play an important role in the development of many chronic diseases, including cancer. Among these factors, obesity and insulin resistance have emerged as major contributors to increased cancer risk. As rates of obesity continue to rise worldwide, researchers are working to understand how excess body fat and metabolic imbalance influence the development and progression of cancer.
Understanding this connection can help individuals make healthier choices and may also guide preventive strategies in modern healthcare.
Obesity is defined as an excessive accumulation of body fat that can negatively affect health. It is often measured using body mass index (BMI), which compares a person's weight to their height. When body fat increases significantly, it does more than simply store energy. Fat tissue becomes metabolically active and begins to produce hormones, inflammatory chemicals, and other substances that can affect the body’s internal balance. These biological changes can create conditions that favor the development of cancer.
One of the key mechanisms linking obesity to cancer is insulin resistance. Insulin is a hormone produced by the pancreas that helps regulate blood sugar levels. After eating, insulin allows cells to absorb glucose from the bloodstream and use it for energy. However, when a person becomes insulin resistant, the body’s cells stop responding properly to insulin. As a result, the pancreas produces more insulin in an attempt to maintain normal blood sugar levels.
Persistently high insulin levels, known as hyperinsulinemia, can have several effects on the body. Insulin is not only a regulator of blood sugar but also acts as a growth-promoting hormone. When insulin levels remain elevated for long periods, they can stimulate cell growth and reduce the natural process of cell death. These conditions may increase the likelihood that abnormal cells will survive and multiply, which can contribute to cancer development.
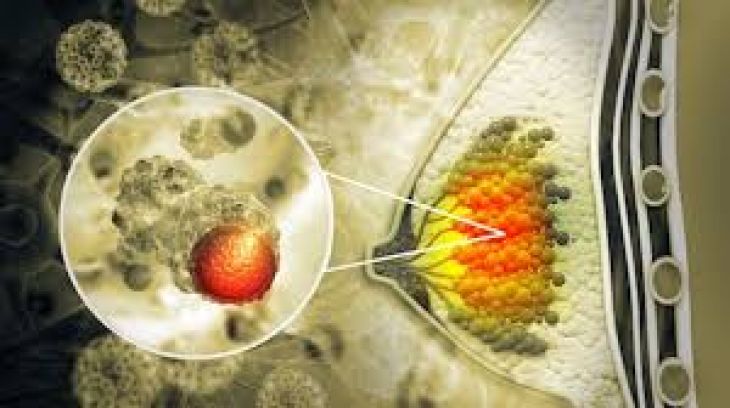
Excess body fat also alters the balance of other hormones in the body. For example, fat tissue produces estrogen, a hormone that plays a role in the growth and development of certain tissues. High levels of estrogen have been linked to an increased risk of several cancers, particularly breast and endometrial cancers. When obesity leads to increased estrogen production, the prolonged hormonal stimulation may promote tumor growth in sensitive tissues.
Another important factor connecting obesity and cancer is chronic inflammation. Fat tissue, especially around the abdomen, releases inflammatory chemicals known as cytokines. These substances can create a constant low-level inflammatory state within the body. Over time, chronic inflammation may damage cells and DNA, increasing the likelihood of mutations that lead to cancer.
Scientists have identified several biological pathways through which obesity and insulin resistance may raise cancer risk:
Elevated insulin levels that stimulate abnormal cell growth.
Increased production of estrogen from excess fat tissue.
Chronic inflammation that damages cells and promotes tumor development.
Higher levels of growth factors that encourage cell division.
Changes in immune system function that weaken the body’s ability to detect abnormal cells.
Accumulation of metabolic stress that affects cellular health.
One of the important growth-related molecules associated with insulin resistance is insulin-like growth factor-1 (IGF-1). This protein plays a role in normal cell growth and development. However, when insulin levels remain high, IGF-1 activity may also increase. Elevated IGF-1 can stimulate cells to divide more rapidly and reduce the natural mechanisms that cause damaged cells to die. This environment allows potentially cancerous cells to survive longer than they should.
Obesity is also associated with changes in the immune system. A healthy immune system is responsible for identifying and destroying abnormal cells before they develop into tumors. However, long-term metabolic stress caused by obesity may weaken immune responses. Inflammatory substances released from fat tissue can disrupt the balance of immune cells, making it harder for the body to recognize and eliminate cancerous cells in their early stages.
Research has shown that obesity is linked to an increased risk of several types of cancer. These include cancers of the breast, colon, liver, pancreas, kidney, and endometrium. The relationship is complex and involves a combination of hormonal, metabolic, and inflammatory changes within the body. While obesity does not guarantee that a person will develop cancer, it significantly increases the likelihood compared to individuals with healthy body weight.
Lifestyle factors often contribute to both obesity and insulin resistance. Diets high in processed foods, sugary beverages, and unhealthy fats can promote weight gain and metabolic imbalance. Physical inactivity also plays a major role, as regular exercise helps regulate blood sugar levels and improves insulin sensitivity. When healthy habits are absent, the body may gradually develop the metabolic conditions that support cancer development.
Fortunately, the connection between obesity, insulin resistance, and cancer also means that lifestyle changes can play a powerful role in prevention. Maintaining a healthy body weight through balanced nutrition and regular physical activity can improve insulin sensitivity and reduce inflammation. These changes help restore metabolic balance and may lower the risk of cancer over time.
Weight loss, even in moderate amounts, can produce significant health benefits. Studies have shown that reducing body weight can improve insulin function, decrease inflammatory markers, and restore hormonal balance. These improvements create an internal environment that is less favorable for cancer development.
Medical research continues to explore new strategies to address metabolic risk factors for cancer. Scientists are studying how certain medications that improve insulin sensitivity may influence cancer risk. At the same time, public health efforts are focusing on promoting healthier lifestyles to reduce obesity rates on a larger scale.
Education and awareness are essential in addressing this issue. Many people still view obesity only as a cosmetic or lifestyle concern, without recognizing its deeper impact on long-term health. Understanding how metabolic health influences cancer risk encourages individuals to take preventive measures early in life.
In conclusion, obesity and insulin resistance play a significant role in increasing cancer risk through a combination of hormonal, metabolic, and inflammatory mechanisms. Excess body fat can disrupt normal biological processes, leading to elevated insulin levels, chronic inflammation, and hormonal imbalances that promote tumor growth. While these risks are serious, they are also largely preventable through healthier lifestyle choices. By maintaining a balanced diet, staying physically active, and managing body weight, individuals can improve metabolic health and potentially reduce their risk of developing cancer in the future.