The Science Behind Metastasis: How Cancer Cells Travel Through Blood and Lymph
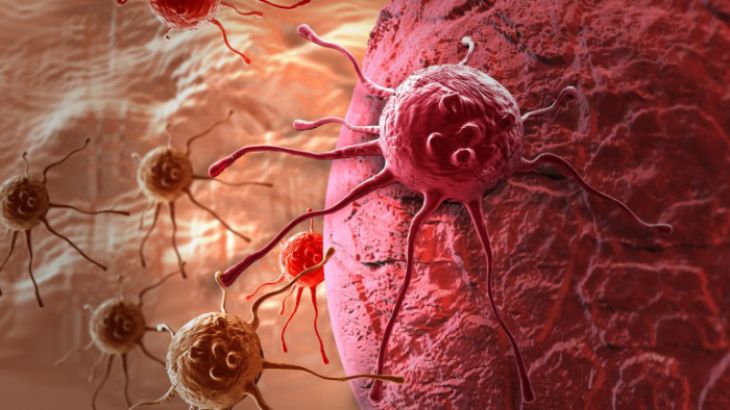
Cancer becomes life-threatening not only because of the original tumor, but because of its ability to spread. This process, known as metastasis, is responsible for the majority of cancer-related deaths. While a primary tumor may sometimes be treated successfully with surgery, radiation, or medication, metastatic cancer is far more complex to control. Understanding how cancer cells travel through the blood and lymphatic systems reveals why metastasis is such a powerful and dangerous biological event.
Metastasis is not a random occurrence. It is a carefully orchestrated sequence of changes that allow cancer cells to detach, survive in circulation, and colonize distant organs. Healthy cells are programmed to remain in their designated tissues. They communicate with neighboring cells and attach firmly to surrounding structures.
Cancer cells, however, acquire genetic and molecular alterations that weaken these attachments and increase mobility.
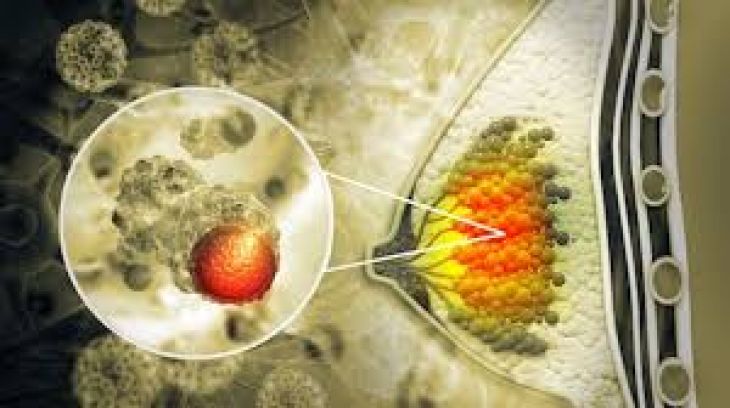
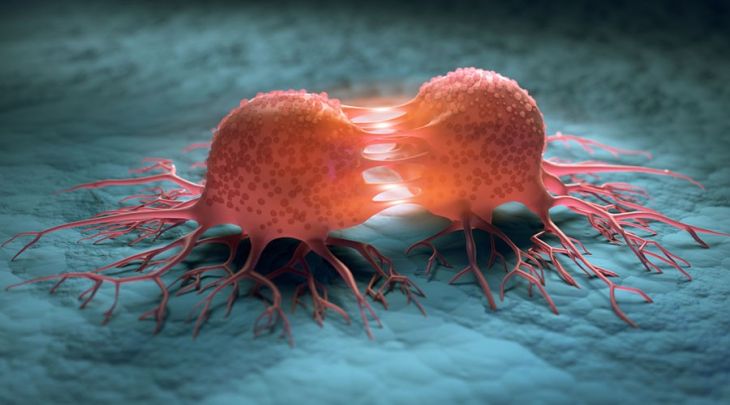
The process begins within the primary tumor. As cancer grows, some cells undergo changes that make them more aggressive. They lose adhesion molecules that normally keep cells bound together. At the same time, they produce enzymes capable of breaking down the extracellular matrix—the supportive framework surrounding tissues. This breakdown allows cancer cells to invade nearby structures.
Once cancer cells invade surrounding tissue, they may enter either blood vessels or lymphatic vessels. Both systems serve as transportation networks within the body. The bloodstream carries oxygen and nutrients, while the lymphatic system plays a key role in immune defense and fluid balance. Unfortunately, these systems can also become pathways for cancer spread.
The metastatic journey typically unfolds in several critical stages:
Local invasion, where cancer cells penetrate nearby tissue.
Intravasation, the entry of cancer cells into blood or lymph vessels.
Survival in circulation, despite immune attacks and physical stress.
Extravasation, the exit of cancer cells from vessels into new tissue.
Colonization, where cells adapt and form a secondary tumor.
Each of these steps presents challenges. The bloodstream, for example, is a hostile environment. Circulating tumor cells face mechanical forces from blood flow and constant surveillance by immune cells. Many cancer cells perish during this stage.
However, some develop survival strategies. They may cluster together, forming protective groups, or bind to platelets, which shield them from immune detection and help them adhere to vessel walls.
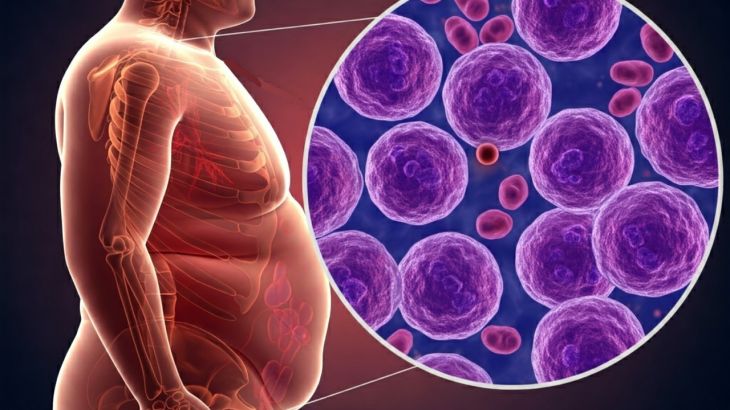
The lymphatic system offers another route for metastasis. Lymph vessels are thinner and more permeable than blood vessels, making it easier for cancer cells to enter. Once inside, cells may travel to nearby lymph nodes. This is why doctors often examine lymph nodes during cancer staging. The presence of cancer in lymph nodes indicates that tumor cells have begun spreading beyond the primary site.
After traveling through circulation, cancer cells must exit the vessels to establish themselves in new tissue. This step, called extravasation, involves attaching to the vessel lining and squeezing through into surrounding tissue. However, arrival alone is not enough. Most circulating tumor cells fail to grow into secondary tumors because the new environment may not support their survival.
The ability of cancer cells to thrive in specific organs relates to what scientists call the “seed and soil” theory. In this concept, cancer cells are the seeds, and distant organs provide the soil. Certain cancers tend to spread to specific organs because the biological environment there supports their growth. For example, some cancers commonly metastasize to the lungs, liver, bones, or brain. Factors such as blood flow patterns, cellular receptors, and local growth signals influence these preferences.
Metastasis also depends heavily on communication between cancer cells and their new surroundings. Cancer cells can manipulate nearby normal cells, including immune cells and connective tissue cells, to create a supportive microenvironment. They may stimulate the formation of new blood vessels, a process called angiogenesis, to supply oxygen and nutrients to the emerging secondary tumor.
Genetic instability within cancer cells plays a central role in metastasis. As tumors grow, they accumulate mutations that increase aggressiveness and adaptability.
Some mutations enhance motility, while others promote resistance to immune attack or cell death. This genetic diversity allows a small subset of cells within the tumor to acquire metastatic potential.
Importantly, metastasis is not an immediate event. It may occur months or years after the initial tumor forms. In some cases, dormant cancer cells remain inactive in distant tissues for extended periods before becoming active again. The reasons for this dormancy and reactivation are areas of ongoing research.
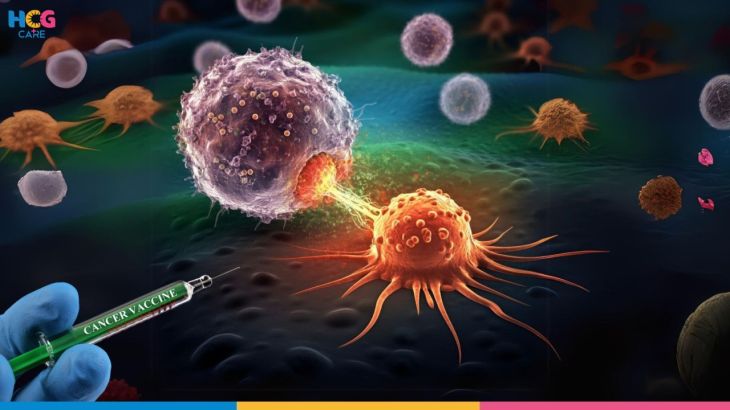
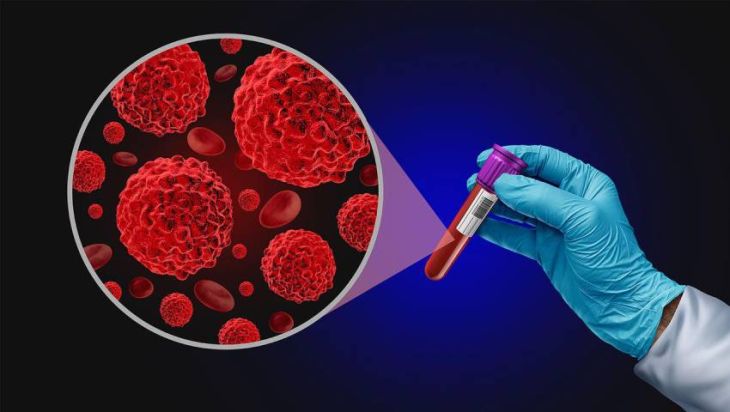
Modern cancer treatments increasingly aim to interrupt the metastatic process. Targeted therapies may block specific molecules involved in invasion or angiogenesis. Immunotherapies enhance the body’s ability to recognize and destroy circulating tumor cells. Researchers are also studying ways to detect circulating tumor cells early, potentially predicting metastasis before secondary tumors become visible on imaging scans.
Despite these advances, metastasis remains one of the greatest challenges in oncology. The complexity of the process, combined with the adaptability of cancer cells, makes it difficult to control completely. However, deeper understanding of the molecular and cellular mechanisms involved continues to inspire new therapeutic strategies.
In conclusion, metastasis is a multi-step biological journey in which cancer cells detach from the primary tumor, travel through blood or lymphatic systems, survive hostile conditions, and establish new tumors in distant organs. It involves local invasion, circulation, immune evasion, and colonization within supportive environments. By unraveling the science behind how cancer cells travel and adapt, researchers are developing more precise methods to prevent and treat metastatic disease. Continued study of this intricate process offers hope for improving survival and reducing the global burden of advanced cancer.